Herpangina is a virus that often hits a child's throat, mainly kids under the age of 5. However, anyone can get it, from babies to teenagers and young grown-ups. This painful infection leads to fevers, and little sores or blisters at the throat's back. It spreads easily, particularly during the summer. Toddlers often get this throat virus because their immune systems haven't matured yet.
Various enteroviruses cause this sickness, with the Coxsackie B virus type being a frequent culprit. Fortunately, this throat virus naturally clears up in children. Its treatment focuses on easing the symptoms. It's worth noting that Herpangina weakens the body and immune system overall. So, bacterial overinfections can occur during the illness, calling for antibiotics.
Herpangina might occur with things like enteroviral rashes or nerve issues. Examples of nerve issues are aseptic meningitis and acute flaccid paralysis. Sometimes, children's viral pharyngitis gets mistaken for group A streptococcal bacterial pharyngitis.
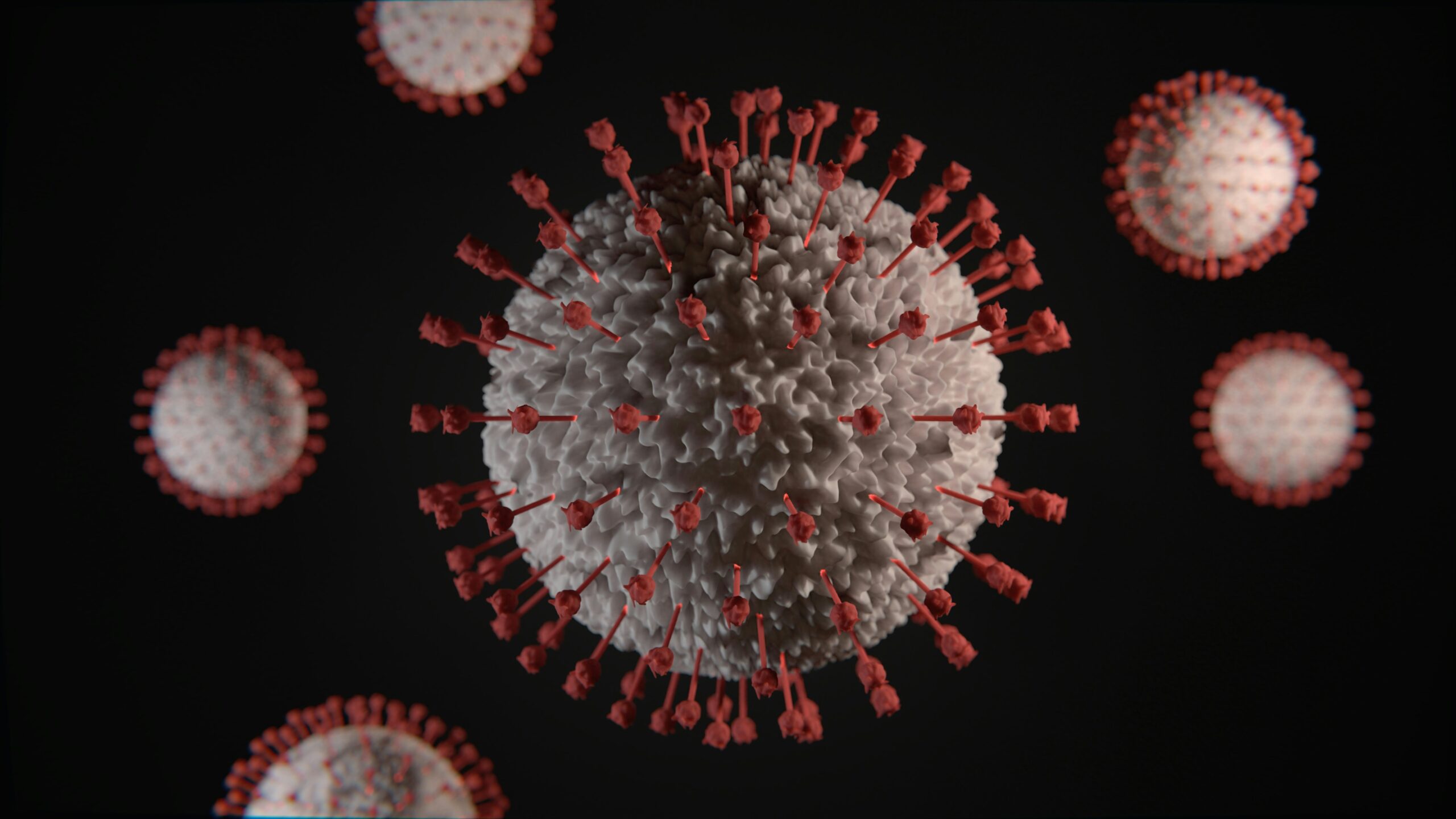
Herpangina resembles angina but with a gentler path. It's a prevalent infection triggered by numerous viruses. Yet, it's infectious and rapidly shared, making it easy for kids to catch it from their friends or siblings. Enteroviruses and echoviruses viruses cause herpangina, most commonly Coxsackie type A![]() . Adenoviruses, rhinoviruses, enteroviruses, or different microorganisms may also be responsible for the ailment.
. Adenoviruses, rhinoviruses, enteroviruses, or different microorganisms may also be responsible for the ailment.
Coxsackie viruses are enteroviruses belonging to the Picornaviridae![]() family. This family includes polioviruses, echoviruses, and Coxsackie viruses. Enteroviruses contain a genome composed of a single strand of RNA, multiply in the gastrointestinal tract, are resistant to stomach acid, and lack a lipid envelope. Despite residing in the gastrointestinal tract, they usually do not cause gastrointestinal infections and diarrhea. Coxsackie virus is named after the town of that name in the United States, where the virus was first isolated. Coxsackie A viruses most often cause herpes pharyngitis, herpangina, respiratory infections, and hemorrhagic conjunctivitis.
family. This family includes polioviruses, echoviruses, and Coxsackie viruses. Enteroviruses contain a genome composed of a single strand of RNA, multiply in the gastrointestinal tract, are resistant to stomach acid, and lack a lipid envelope. Despite residing in the gastrointestinal tract, they usually do not cause gastrointestinal infections and diarrhea. Coxsackie virus is named after the town of that name in the United States, where the virus was first isolated. Coxsackie A viruses most often cause herpes pharyngitis, herpangina, respiratory infections, and hemorrhagic conjunctivitis.
Enterovirus infections are common. They frequently show no signs or mimic symptoms of a sudden sickness with fever and effects similar to the flu. Rashes of different shapes and forms often mark these infections. Newborns and infants, whose immune defenses are not yet fully developed, have a higher risk of experiencing more serious cases of the disease.
Germs that cause herpangina, a sore throat, can travel through droplets![]() and traces of feces
and traces of feces![]() . Infections from the Coxsackie virus, a common cause of this illness, increase in the summer and fall seasons. Outbreaks of these germs are often seen in places like kindergartens and daycare places.
. Infections from the Coxsackie virus, a common cause of this illness, increase in the summer and fall seasons. Outbreaks of these germs are often seen in places like kindergartens and daycare places.
The germs can spread through the air or by touching someone sick. They first enter your body in your guts and multiply there. Then, they leave your body, potentially infecting others. Not being clean can make getting this sickness more likely. So, things that make you more likely to get herpangina are:

Young age – Kids often get viral pharyngitis. They haven't built up a strong immune system yet. It can take seven years for their immune system to mature fully. That leaves them open to germs, especially in the fall and winter. Other things make them susceptible to herpangina, too. They're around other kids in school and kindergarten. Plus, they're not always the best at staying clean.
Contact with an infected person – Herpangina is something you can catch. If you're near someone who's sick, it's risky. Teachers, parents, you could all get it, even from an object that a sick person touched. That's why washing your hands is the best way to protect yourself. Do it often and at key times. Before you eat, after using the toilet, after a sneeze, and after changing a diaper. Making sure to clean any dirty surfaces is a good idea, too.
Being in public places – Certain places have a higher chance of catching herpangina. These places are usually public, like schools or kindergartens. The virus is tough; it resists many chemical agents and survives even in sewage. You can get it from an infected person's food or droplets or through water. Yes, even swimming pools can be enterovirus hotspots.
Inadequate hygiene – Not cleaning properly can cause sickness to spread. Unwashed hands can transfer germs to your mouth and stomach. Keeping clean can prevent illness. In one study, improved hand hygiene was observed to curb a herpangina outbreak. It was an infection triggered by the human enterovirus. Parents answered surveys regarding their children's cleanliness and exposure. This significantly reduced the risk.

Herpangina manifests itself similarly to other types of tonsillitis, so it includes systemic symptoms. In addition, it also has specific symptoms that help in the diagnosis of herpangina. Generally, Herpangina starts subtly. Usually, we see some signs two days before the disease shows up fully. Then, pharyngitis-like symptoms come into play. Another name for Herpangina is hand-foot-mouth disease. This name tells us that this disease shows up as little fluid-filled blisters. These blisters appear on the hands, feet, and buttocks. Plus, you'll notice some classic Herpangina marks in the mouth. Symptoms might be:
Flu-like symptoms – Herpangina first appears like a normal flu, showing symptoms like high-grade fever![]() , muscle pain, throat soreness, cough, and a runny nose. These signs show up around two days before herpangina fully manifests. The disease does not cause all these symptoms in everyone; each person's experience can vary. In some cases, herpangina runs completely asymptomatic.
, muscle pain, throat soreness, cough, and a runny nose. These signs show up around two days before herpangina fully manifests. The disease does not cause all these symptoms in everyone; each person's experience can vary. In some cases, herpangina runs completely asymptomatic.
Respiratory symptoms – People with herpangina often experience breathing problems and heightened blood pressure. This can be due to sickness, high temperatures, or stress, potentially lifting blood pressure short-term. Such changes may spark perspiration, heart flutters, or breathlessness. Sometimes, an enterovirus infection triggers these breathing issues. It can lead to respiratory diseases.
Gastrointestinal symptoms – Herpangina sometimes causes tummy troubles. This could mean feeling unwell, tossing your cookies, having a bellyache, or running to the bathroom often. It may appear similar to a fierce tummy bug. However, remember, tummy trouble isn't a typical symptom for those facing herpangina. More research is needed to clarify symptoms such as diarrhea![]() caused by various serotypes of enteroviruses.
caused by various serotypes of enteroviruses.
Rash and herpes – Kids dealing with hand, foot, and mouth disease (HFMD) or herpangina might notice early signs like a rash or sores. These sores typically appear on their hands, feet, bottoms, and knees. Some kids might even see this rash happening in other parts of their bodies. The rash can look different ways. It might be scaly, bumpy, fluid-filled, pimple-like, or blister-like. These variations happen because of the specific type of virus they have.
Throat ulceration – Herpangina often causes throat soreness and red sores. It's like having a sore throat. Sometimes the soft part of the roof of your mouth can show red spots and ulcers. However, this can also not happen. Sometimes, small bumps may appear, similar to herpangina, but no blisters or sores. Herpangina often causes pain, targeting areas such as tonsils, soft palate, and throat backside. Occasionally, sores might appear on the mouth's sides or the back of the tongue.
Lymph nodes can enlarge – It's not uncommon for doctors to find an expansion in a patient's lymph nodes during routine exams. These lymph nodes are scattered throughout the body and are generally found in clusters. You'll see the largest clusters under the jaw and in your neck region. Often, during viral infections, these neck lymph nodes might swell up. This is due to an increase in lymphocytes and other types of inflammation cells in your blood.
Leukopenia – Herpangina can also affect the amount of blood components![]() . Leukopenia is a condition where white blood cell levels drop. A slight deficiency usually has no symptoms. On the other hand, more considerable deficiencies may be experienced as a sub-febrile state and recurrent respiratory infections. Various infections are among the most common causes of leukopenia, especially at the beginning of their development.
. Leukopenia is a condition where white blood cell levels drop. A slight deficiency usually has no symptoms. On the other hand, more considerable deficiencies may be experienced as a sub-febrile state and recurrent respiratory infections. Various infections are among the most common causes of leukopenia, especially at the beginning of their development.
Drooling – Herpangina in little kids can cause an unusual amount of drool, not because they're teething. Kids with this illness often don't want to eat. Even swallowing drinks and semi-solid foods can be tough for them. This unwillingness towards food and drink may make them weak and dehydrated.

A doctor can identify herpangina through a patient's narrative and symptom check. No extra scans or lab tests are needed if the case isn't critical. We occasionally run these tests to exclude the likelihood of other diseases. Enterovirus tests are available to verify the virus's presence in the body. Yet, due to the virus's extended culture time, these tests are rarely used. The extended waiting period can last about a week, making the test useless. Instead, we use these diagnostic methods:
Polymerase Chain Reaction (PCR) Testing – This test quickly finds enteroviruses and does it well. It sniffs out these viruses in places like skin ulcers, fluid-filled bumps, or stool. It's called molecular testing. It finds the viruses in the DNA![]() . But remember, don't brush your teeth if you're about to do a throat swab.
. But remember, don't brush your teeth if you're about to do a throat swab.
Immunoenzymatic (ELISA) Tests – Immunoenzymatic (ELISA) tests are also available for the diagnosis of herpangina. The Elisa test involves the detection of specific proteins in the test material. These medical tests are generally less sensitive than PCR and should only be used when PCR is unavailable. This technique is most often used to confirm the presence of single antigens![]() in the diagnosis of autoimmune disorders and to monitor treatment progress.
in the diagnosis of autoimmune disorders and to monitor treatment progress.

It's important to consider other illnesses that could cause the same symptoms as herpangina. This disease looks the same as a few other childhood illnesses![]() . We need to cross out other diseases and conditions before confirming a herpangina diagnosis. This is super important because different treatments are needed for bacterial infections. Here are some diseases that could be confused with herpangina:
. We need to cross out other diseases and conditions before confirming a herpangina diagnosis. This is super important because different treatments are needed for bacterial infections. Here are some diseases that could be confused with herpangina:
Measles – Measles is a disease passed on by a virus. It causes symptoms like high fever, dry cough, light sensitivity, and a specific type of rash. This rash often looks like many small, grayish spots. Occasionally, measles might bring about signs like loose stools, swollen glands, and not wanting to eat. These symptoms might look like another condition, herpangina.
Chickenpox – Chickenpox often affects kids. The Varicella-zoster virus causes it. Typical signs are fever, feeling off, and a patchy skin rash with bumps filled with liquid. When grown-ups get chickenpox, it's often harsher. Its symptoms might get mixed up with herpangina symptoms.
Erythema multiforme – Erythema multiforme is a kind of sensitivity reaction. Triggers like infections, medicines, or chemicals can cause it. The intensity can vary. People with Erythema multiforme may have red patches or blisters on the skin, differing in severity. It can be wrongly identified as herpangina due to its similar appearance.
Eczema herpeticum – There's a unique herpes infection named eczema herpeticum. Babies, especially those 6 to 12 months old, commonly get this. Yet, it can happen to adults and older kids, just not as much. Here's how it works. The virus subtly lands on the lips or mouth. Then, little skin spots appear on the face and scatter across the body. A tell-tale sign is a high fever. Interestingly, it can also resemble another condition, the herpangina.
Kawasaki disease – Kawasaki disease moves fast and usually hits youngsters. It swells the tubes that transport blood in the body. The main signs? A big fever, throat hurting, eyes glowing red, a strange-looking tongue, and puffiness in the toes and fingers. Baddies like germs, viruses, and poisons might start it. The body's defense system then goes into overdrive. Its signs can look a lot like herpangina.
Rocky Mountain spotted fever – A bacteria named R. rickettsii, most commonly found on forest ticks causes a disease known as Rocky Mountain spotted fever. This disease's signs are unclear and could easily be confused with food poisoning. Just like in herpangina, one noticeable sign here can be a skin rash. It's a light red rash that can develop into a bleeding reaction. The rash first shows up on the bends of wrists and ankles, and then, over time, it spreads to the arms, legs, back, and chest.
Drug eruption – Finding the root cause of a drug reaction is critical. Remembering to record the drug that sparked such a reaction in a patient's files is key, too. Diverse medications can trigger a range of side effects. Skin rashes are one common outcome. The look of skin sores can mimic many infectious diseases, like herpangina.

Herpangina often takes a mild course, but seeing a doctor for personal treatment is best. Patients benefit from solitude in airy, clean spaces to stop the spread of infection. It's a disease that resolves on its own. Treatment is mostly supportive. Relief from symptoms comes first. Antibiotics don't work on viral infections. Rather, here are some treatments we can use:
Oral hygiene – Keeping your mouth clean matters a lot. For a sickness called herpangina, it's suggested that patients wash their mouths with salt water after food. Small kids can clean their mouths with the usual saline if they find their mouths rinsing hard. No saline? Saltwater is a good substitute. Staying hydrated is key in treating herpangina. However, applying medication with stuff like lidocaine or diphenhydramine isn't typically advised. Why? The chance of harmful effects and the absence of suitable research on their effectiveness.
Hydration – Herpangina patients could get dehydrated. Kids with a high fever and trouble eating need enough fluids with electrolytes. We need to watch these patients because problems can arise carefully. High fever might result in seizures in younger kids; quick action is required.
Antipyretic treatment – Herpangina often shows up as a high fever. When the body temp goes over 101.3°F/38.5°C![]() , fever reducers like ibuprofen or acetaminophen can help. Other methods include a cool cloth on the forehead, using patches that bring down fever, or resting with ice near the head.
, fever reducers like ibuprofen or acetaminophen can help. Other methods include a cool cloth on the forehead, using patches that bring down fever, or resting with ice near the head.
Antiviral treatment – For herpangina, there isn't a designated antiviral remedy. We mostly manage its symptoms. Wide-ranging antiviral medicines that include acyclovir and gancyclovir don't aid. Some suggest an i********n alfa spray. Its local application might aid as it can modulate the immune response and fight viruses. This is because i********n alfa helps keep the mucus surfaces of the body immune to infections.

Herpangina is generally a benign condition that resolves independently, posing little danger. Viral infections often reduce immunity so that bacterial superinfections can happen afterward. However, it should be remembered that some causative microorganisms, such as enterovirus, can cause serious complications. Such patients are usually considered critical and require hospitalization. In some cases, intensive care unit care is recommended. Complications of herpangina include brainstem inflammation![]() , acute flaccid paralysis
, acute flaccid paralysis![]() , aseptic meningitis
, aseptic meningitis![]() , and myocarditis
, and myocarditis![]() .
.
Herpangina is a mild throat infection, often caused by different viruses. It's widespread and highly contagious, so kids can easily catch it from their friends or siblings. Enteroviruses and echoviruses are often responsible, especially the Coxsackie group A virus. Other viruses might cause it, too. Germs causing herpangina, a sore throat, spread through tiny water droplets and even feces. The Coxsackie virus causes many herpangina cases, more during summers and autumn.
Schools for younger kids see germ outbreaks often. Herpangina symptoms are like any other tonsillitis and come with health issues. Different symptoms can help doctors identify herpangina. Usually, patients show subtle signs a couple of days before they feel sicker. Then, symptoms of a sore throat trouble them.
A doctor can diagnose herpangina by listening to the patient's story and checking their symptoms. They usually don't need extra tests if the case isn't severe. Even though it's mild, patients should visit a doctor. Staying alone in clean, airy rooms helps avoid the spread. Mostly, the disease goes away on its own, and treatments aid relief from symptoms first. Since it's a virus, antibiotics won't help.